Panic attack
| Panic attack | |
|---|---|
 | |
| A depiction of someone experiencing a panic attack being reassured by another person | |
| Specialty | Psychiatry |
| Symptoms | Periods of intense fear, palpitations, sweating, shaking, shortness of breath, numbness[1][2] |
| Complications | Self-harm, suicide,[2] agoraphobia |
| Usual onset | Over minutes[2] |
| Duration | Seconds to hours[3] |
| Causes | Panic disorder, social anxiety disorder, post-traumatic stress disorder, drug use, depression, medical problems[2][4] |
| Risk factors | Nicotine, caffeine, cannabis, psychological stress[2] |
| Diagnostic method | After other possible causes excluded[2] |
| Differential diagnosis | Hyperthyroidism, hyperparathyroidism, heart disease, lung disease, drug use, dysautonomia[2] |
| Treatment | Counselling, medications[5] |
| Medication | Acute: Benzodiazepines[6] Preventative: Antidepressants, anxiolytics |
| Prognosis | Usually good[7] |
| Frequency | 3% (EU), 11% (US)[2] |
Panic attacks are sudden periods of intense fear and discomfort that may include palpitations, otherwise defined as a rapid, irregular heartbeat, sweating, chest pain or discomfort, shortness of breath, trembling, dizziness, numbness, confusion, or a sense of impending doom or loss of control.[1][2][8] Typically, these symptoms are the worst within ten minutes of onset and can last for roughly 30 minutes, though they can vary anywhere from seconds to hours.[3][9] While they can be extremely distressing, panic attacks themselves are not physically dangerous.[7][10]
The Diagnostic and Statistical Manual V (DSM-5) defines them as "an abrupt surge of intense fear or intense discomfort that reaches a peak within minutes and during which time four or more of the following symptoms occur." These symptoms include, but are not limited to, the ones mentioned above.[11]
Panic attacks function as a marker for assessing severity, course, and comorbidity (the simultaneous presence of two or more diagnoses) of different disorders, including anxiety disorders. Hence, panic attacks can be applied to all disorders found in the DSM.[12]
Panic attacks can be caused by a identifiable source, or they may happen without any warning and without a specific, recognizable situation.[2]
Some known causes that increase the risk of having a panic attack include medical and psychiatric conditions (e.g., panic disorder, social anxiety disorder, post-traumatic stress disorder, substance use disorder, depression), substances (e.g., nicotine, caffeine), and psychological stress.[2][4]
Before making a diagnosis, physicians seek to eliminate other conditions that can produce similar symptoms, such as hyperthyroidism (an overactive thyroid), hyperparathyroidism (an overactive parathyroid), heart disease, lung disease, and dysautonomia, disease of the system that regulates the body's involuntary processes.[2][13]
Treatment of panic attacks should be directed at the underlying cause.[7] In those with frequent attacks, counseling or medications may be used, as both preventative and abortive measures, ones that stop the attack while it is happening.[5] Breathing training and muscle relaxation techniques may also be useful.[14]
Panic attacks often appear frightening to both those experiencing and those witnessing them, and often, people tend to think they are having heart attacks due to the symptoms.[15] However, they do not cause any real physical harm.
Previous studies have suggested that those who suffer from anxiety-related disorders (e.g., panic disorder) are at higher risk of suicide.[16]
In Europe, approximately 3% of the population has a panic attack in a given year, while in the United States, they affect about 11%.[2] Panic attacks are more prevalent in females than males and often begin during puberty or early adulthood.[2] Children and older adults are less commonly affected.[2]

Signs and symptoms
[edit]When people experience a panic attack, it usually comes on very suddenly and unexpectedly with a wide range of symptoms that tend to last, on average, a few minutes.[17] Typically, the symptoms of panic attacks reach their worst intensity in the first minute, before subsiding over the course of several minutes.[18] During this time, people often feel intense fear that something catastrophic will happen despite there being no immediate danger.[1] The frequency of panic attacks vary between individuals, with some people experiencing a panic attack as frequently as every week, while others could have one panic attack per year.[19] The features that help define a panic attack are the collection of symptoms that accompany a panic attack as well as the fact that a panic attack occurs unprompted; meaning there is usually no triggering event that causes a panic attack.[19]
Panic attacks are associated with many different symptoms, with a person experiencing at least four of the following symptoms: increased heart rate, chest pain, palpitations (i.e. feeling like your heart is pounding out of your chest), difficulty breathing, choking sensation, nausea, abdominal pain, dizziness, lightheadedness (i.e. feeling like you might pass out), numbness or tingling (also called paresthesias), derealization (i.e. feeling detached from reality, like the events occurring are not real), depersonalization (i.e. feeling disconnected from your body or thoughts), fear of losing control, and fear of dying.[19]
These physical symptoms are interpreted with alarm in people prone to panic attacks. This results in increased anxiety and forms a positive feedback loop, meaning that the more a person experiences symptoms associated with a panic attack, the more they experience feelings of anxiety which serve to worsen their panic attacks.[20] Panic attacks are distinguished from other forms of anxiety by their intensity and their sudden, episodic nature.[21]
Chest pain
[edit]People can experience a wide range of symptoms during their panic attacks; they tend to be very intense and frightening and the common symptoms of difficulty breathing and chest pain can sometimes cause people to believe they are having a heart attack, leading them to go to the emergency department.[18] Because chest pain and difficulty breathing are commonly symptoms of some sort of heart disease (such as a heart attack), there is medical importance in ruling out life-threatening reasons for their symptoms.[22] A heart attack (also called a myocardial infarction) occurs when there is a blockage in the arteries going to the heart, causing less blood to get to the heart tissue, and ultimately causing the heart tissue to die.[22] This will be evaluated in the emergency department with an EKG (i.e. a picture of the electrical activity of the heart) and by measuring a hormone called troponin, which is released from the heart tissue during times of stress on the tissue.[22]
Causes
[edit]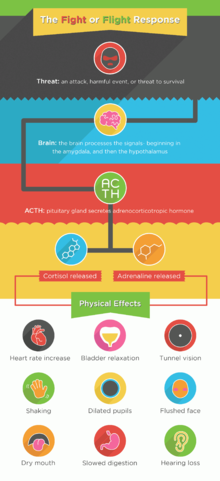
Panic attacks can be caused by a mix of factors. Biological factors that may lead to panic attacks include psychiatric disorders such as post-traumatic stress disorder and obsessive–compulsive disorder, heart conditions, low blood pressure, and an overactive thyroid. Imbalance of the norepinephrine system, which is responsible for coordinating the body's fight-or-flight response has been linked to panic attacks as well.[23]
Panic disorder tends to arise in early adulthood, though it can occur at any age. It is more common in women and usually arises more in individuals with above-average intelligence.[24][25] Research involving identical twins has shown that if one twin has an anxiety disorder, the other is likely to have one too.[26]
Panic attacks may also occur due to short-term stressors. Major personal losses, like the end of a romantic relationship, life transitions, such as jobs, moving, etc. and significant life changes may all trigger a panic attack. Individuals who are naturally anxious, need a lot of reassurance, worry excessively about their health, have an overcautious view of the world, and have cumulative stress are more likely to experience panic attacks.[21][27] For teenagers/adolescents, social transitions, including changes in classes and schools may also be a contributing factor.[28]
People often experience panic attacks as a direct result of exposure to specific fears or phobias. A situation can become associated to panic if someone has had a previous reaction before in similar contexts.
Substances may also induce panic attacks. For example, discontinuation or reduction in the dose of a drug (drug withdrawal) without tapering can cause a panic attack. Other substances that are commonly known to be associated with panic attacks include marijuana and nicotine.[29][30]
Panic disorder
[edit]People who have repeated, persistent attacks or feel severe anxiety about having another attack are said to have panic disorder. Panic disorder is strikingly different from other types of anxiety disorders in that panic attacks are often sudden and unprovoked.[31] However, panic attacks experienced by those with panic disorder may also be linked to or heightened by exposure to certain places or situations, making daily life difficult.[32]
If a person has repeated and unexpected panic attacks, this could be a potential sign of panic disorder. According to the DSM-5, panic disorder can be diagnosed if a patient has not only recurrent panic attacks but also experiences at least a month of anxiety or worry about having additional attacks. This concern may lead to the person to modify their behavior to avoid situations that triggered the attack. Panic disorder cannot be diagnosed if the patient has another disorder that is causing the panic attacks (e.g. social anxiety disorder).[20]
Patients affected by panic disorder can struggle with depression and a diminished quality of life. Compared to the general population, they are also at increased risk for substance abuse and addiction.[20]
Agoraphobia
[edit]Panic disorder frequently presents with agoraphobia, which is an anxiety disorder where the individual presents with fear of a situation from which they cannot leave or escape, especially if a panic attack occurs. People who have had a panic attack in certain situations may develop phobias of these situations and begin to take measure to avoid them. Eventually, the pattern of avoidance and level of anxiety about another attack may reach the point where individuals with panic disorder are unable to drive or even step out of the house, preferring the comfort of remaining in a safe and known place.[33] At this stage, the person is said to have panic disorder with agoraphobia.[34]
In Japan, people who exhibit extreme agoraphobia to the point of becoming unwilling or unable to leave their homes are referred to as Hikikomori.[35] This term is used to describe both the person and the phenomenon. After first being defined by the Japanese Ministry of Health, Labor, and Welfare, a national research task force refined the definition as “the state of avoiding social engagement (e.g., education, employment, and friendships) with generally persistent withdrawal into one’s residence for at least six months as a result of various factors."[36]
Pathophysiology
[edit]
When panic attacks occur, people experience the sudden onset of fear and anxiety in the setting of no actual perceived threat (ex. your mind believes there is something threatening your wellbeing, but there is nothing actual life-threatening occurring). This fear-based response leads to a release of a hormone called adrenaline (also known as epinephrine), which brings about the fight-or-flight response. One part of our nervous system is made up of both the sympathetic nervous system, which is responsible for the fight-or-flight response, and the parasympathetic nervous system, which is responsible for the rest-and-digest response.[37] The sympathetic nervous system prepares our body for strenuous physical activity (i.e. fight or flight) by affecting different bodily functions such as increasing heart rate, increasing breathing, sweating and many others, leading to the physical symptoms that accompany a panic attack.[37] The reason panic attacks occur remain unclear; there are several different ideas for why some people experience panic attacks while others don't. The current theories include the fear network model, theory of acid-base disturbances in the brain, and irregular activity of the amygdala (i.e. the part of the brain responsible for controlling emotions, such as fear, and identifying threats).[38][39][40][41]
Fear network model
[edit]The fear network model hypothesizes that parts of our brain responsible for controlling the fear response that is created by the area of the brain where the amygdala is located (called the limbic system) is unable to control the fear sufficiently, leading to panic attacks.[41] It is thought that dysfunction of the area responsible for controlling fear could be due to stress experienced in childhood, along with a genetic component as well.[41] In summary, the fear network model states that the network in our brains responsible for responding to fear and then controlling that fear is not working properly, creating the inability for our brains to control fear that is occurring without any sort of external threat, leading to panic attacks.[41]
Acid-base disturbances theory
[edit]This theory suggests that there is a part of the amygdala that is able to identify when the pH in our brain decreases, i.e. becomes more acidic.[38] This part of the amygdala is called the acid-sensing ion channel.[38] Since panic attacks typically occur without an obvious external trigger (meaning there is usually nothing life-threatening happening to cause a panic attack), studies have shown that panic attacks may be caused by internal triggers.[39] One such internal trigger is the amygdala sensing acidosis, which can be caused by inhaling CO2 (carbon dioxide).[38][39] In fact, one study has shown that people with a history of panic attacks had disturbances in their pH level minutes before having a panic attack.[39]
Another theory, called the false suffocation alarm theory, is associated with the idea of acid-base imbalances in the amygdala.[38][39] In this theory, inhalation of CO2 causes accumulation of acid in the blood and difficulty breathing, leading our brain to believe that we are suffocating, causing fear and panic.[38] Studies have shown that inhaling CO2 can cause fear in people who do not have any prior history of panic attacks.[38] This information has allowed scientists to suggest that panic attacks could be caused by our brain's inability to stop alarm signals that make us feel like we're suffocating.[38]
Amygdala dysfunction theory
[edit]The amygdala in the human brain has several distinct sections that are responsible for our fear response. This theory suggests that problems in any of these brain areas or the connections between them could lead to excessive fear responses, like panic attacks. Studies have shown that in both animal and human subjects with a history of panic attacks, the amygdala is hyperactive with decreased volume when compared to the control. Another role the amygdala may play in panic attacks is decreased inhibition of amygdalar activity (i.e. the amygdala is not being shut down like it normally should), leading to increased levels of anxiety. A link between childhood traumatic experiences, as well as genetic abnormalities, has been found in those with a dysfunctional amygdala.[40]
Neurotransmitter imbalances
[edit]Many neurotransmitters are affected when the body is under the increased stress and anxiety that accompany a panic attack. Some include serotonin, GABA (gamma-aminobutyric acid), dopamine, norepinephrine, and glutamate.[42]
An increase of serotonin in certain pathways of the brain seems to be correlated with reduced anxiety. More evidence that suggests serotonin plays a role in anxiety is that people who take selective serotonin reuptake inhibitors (SSRIs) tend to feel a reduction of anxiety when their brain has more serotonin available to use.[42]
The main inhibitory neurotransmitter in the central nervous system (CNS) is GABA. This neurotransmitter acts by inhibiting, or blocking nerve signals, which is very helpful in anxiety. In fact, medications that increase GABA in the brain, such as benzodiazepines and barbiturates help with reducing anxiety almost immediately.[42]
Dopamine's role in anxiety is not well understood. Some antipsychotic medications that block dopamine production have been proven to treat anxiety. However, this may be attributed to dopamine's tendency to increase feelings of self-efficacy and confidence, which indirectly reduces anxiety. On the other hand, other medications that increase dopamine levels have also been found to improve anxiety.[42]
Many physical symptoms of anxiety, such as rapid heart rate and hand tremors, are regulated by norepinephrine. Drugs that counteract norepinephrine's effect may be effective in reducing the physical symptoms of a panic attack.[42] On the other hand, some medications that raise overall norepinephrine levels, like tricyclics and serotonin-norepinephrine reuptake inhibitors (SNRIs), can be effective for treating panic attacks over the long term by reducing the sudden increases in norepinephrine that happen during a panic attack.[43]
Because glutamate is the primary excitatory neurotransmitter involved in the central nervous system (CNS), it can be found in almost every neural pathway in the body. Glutamate is likely involved in conditioning, which is the process by which certain fears are formed, and extinction, which is the elimination of those fears.[42]
Cardiac mechanism
[edit]People who have been diagnosed with panic disorder have approximately double the risk of heart disease.[44] Panic attacks can cause chest pain by affecting blood flow in arteries of the heart. During a panic attack, the body's stress response is triggered which can cause the small vessels of the heart to tighten, leading to chest pain. The body's nervous system and rapid breathing during a panic attack can cause spasming of the arteries of the heart (also known as vasospasm). This can reduce blood flow to the heart, causing damage to heart tissue and chest pain, despite normal heart scans.[45]
In individuals with a history of coronary artery disease, panic attacks and stress can make chest pain worse by increasing the heart's need for oxygen. This occurs because increased heart rate, blood pressure, and stress responses (i.e. the sympathetic nervous system) puts more strain on the heart.[45][46][47]
Diagnosis
[edit]According to the DSM-5, a panic attack is part of the diagnostic class of anxiety disorders.[48] DSM-5 criteria for a panic attack is defined as "an abrupt surge of intense fear or intense discomfort that reaches a peak within minutes and during which time four or more of the following symptoms occur":[48]
|
While some patients go to the emergency department due to their physical symptoms, there is no laboratory or imaging test used to diagnose panic attacks, it is a purely clinical diagnosis (i.e. the doctor uses their experience and expertise to diagnose panic attacks) once other more life-threatening diseases have been ruled-out.[19] Due to the physical symptoms that occur with a panic attack, people tend go to the emergency department for further evaluation, however, those who are experiencing panic attacks that are affecting their health and wellness should be seen by a mental health professional, such as a therapist or psychiatrist.[19] Screening tools, such as the Panic Disorder Screener (PADIS), can be used to detect possible cases of panic disorder and suggest the need for a formal diagnostic assessment with a psychiatrist for further evaluation.[49]
Treatment
[edit]Panic disorder is usually effectively managed with a variety of interventions, including psychological therapies and pharmacological treatment with medication.[50][21] The focus on management of panic disorder involves reducing the frequency and intensity of panic attacks, reducing anticipatory anxiety and agoraphobia, and achieving full remission.[51]
If a patient is experiencing a panic attack, most will resolve spontaneously within a course of 20 to 30 minutes without interference.[citation needed] However, benzodiazepines, specifically alprazolam and clonazepam, are frequently prescribed for panic disorder due to their quick onset of action and good tolerability and can thus be used as a way to end a current, on-going attack.[52] Additionally, deep breathing techniques and relaxation can be used and are found to be helpful while the person is experiencing a panic attack or immediately after as a way to calm oneself.[51] Some maintaining causes include avoidance of panic-provoking situations or environments, anxious/negative self-talk ("what-if" thinking), mistaken beliefs ("these symptoms are harmful and/or dangerous"), and withheld feelings.
Cognitive-behavioral therapy has the most complete and longest duration of effect, followed by specific selective serotonin reuptake inhibitors.[53] A 2009 review found positive results from therapy and medication and a much better result when the two were combined.[54]
Lifestyle changes
[edit]Growing research suggests that along with standardized medical treatments, lifestyle changes can help alleviate some of the most common mental health conditions.[55] Because of this, there has been a growing emphasis on the potential of lifestyle interventions and non-pharmacological methods for anxiety.[56] These lifestyle interventions include, but are not limited to, focusing on physical activity, substance avoidance, and relaxation techniques.
Exercise, especially aerobic, have become an alternative method for decreasing symptoms of anxiety and panic. Other more relaxing forms, such as yoga and tai chi, have also had similar effects in improving anxiety and can also be used as adjunctive therapy. Numerous studies have determined that exercise is inversely related to anxiety symptoms, thus as physical activity increases, levels of anxiety seem to decrease. There is evidence that suggests that this effect is correlated to the release of exercise-induced endorphins and the subsequent reduction of the stress hormone, cortisol.[57] One thing to keep in mind is that with exercise, often comes increased respiration rate. This can lead to hyperventilation and hyperventilation syndrome, which mimics symptoms of a heart attack, thus inducing a panic attack,[58] so it is important to pace the exercise regimen accordingly.[59]
Substance avoidance can be important in reducing anxiety and panic symptoms, as many substances can cause, exacerbate, or mimic symptoms of panic disorder. For example, caffeine has been known to have anxiety and panic-inducing properties that can especially present in those who are more susceptible to panic attacks.[60] Anxiety and panic can also temporarily increase during withdrawal from caffeine and various other drugs and substances.[61]
Meditation may also be helpful in the treatment of panic disorders.[62] Muscle relaxation techniques are useful to some individuals as well. These can be learned using recordings, videos, or books. While muscle relaxation has proved to be less effective than cognitive-behavioral therapies in controlled trials, many people still find at least temporary relief from muscle relaxation.[27]
Breathing exercises
[edit]Irregularities in breathing, including hyperventilation and shortness of breath, are key features of anxiety and panic: "dysfunctional breathing is the hallmark of anxiety disorders."[63] Hyperventilation syndrome occurs when an individual experiences deep, quick-paced breathing, eventually affecting blood flow to the brain and altering conscious awareness.[63]
It has been shown that several various breathwork techniques can reduce symptoms in patients diagnosed with anxiety disorders. By managing and focusing on breathing, individuals with anxiety experience less tension and stress in their muscles, as well as a diminished stress response.[63] Breathing retraining exercise helps to rebalance the oxygen and CO2 levels in the blood, improving cerebral blood flow.[64] Capnometry, which provides exhaled CO2 levels, may help guide breathing.[65][66]
David D. Burns recommends breathing exercises for those with anxiety. One such breathing exercise is a 5-2-5 count. Using the stomach (or diaphragm)—and not the chest—inhale (feel the stomach come out, as opposed to the chest expanding) for 5 seconds. As the maximal point at inhalation is reached, hold the breath for 2 seconds. Then slowly exhale, over 5 seconds. Repeat this cycle twice and then breathe 'normally' for 5 cycles (1 cycle = 1 inhale + 1 exhale). The point is to focus on breathing and relax the heart rate.[67]
Although breathing into a paper bag was a common recommendation for short-term treatment of symptoms of an acute panic attack,[68] it has been criticized as inferior to measured breathing.[69][70]
Therapy
[edit]According to the American Psychological Association, "most specialists agree that a combination of cognitive and behavioral therapies are the best treatment for panic disorder. Medication might also be appropriate in some cases."[71] The first part of therapy is largely informational; many people are greatly helped by simply understanding exactly what panic disorder is and how many others experience it. Many people with panic disorder are worried that their panic attacks mean they are "going crazy" or that the panic might induce a heart attack. Cognitive restructuring helps people to replace those thoughts with more realistic, positive ways of viewing the attacks.[72] Avoidant behavior, such as what is seen in patients with agoraphobia, is one of the key aspects that prevent people with frequent panic attacks from functioning healthily.[27] Exposure therapy,[73] which includes repeated and prolonged confrontation with feared situations and body sensations, helps weaken anxiety responses to panic-inducing external and internal stimuli.
In deeper-level psychoanalytic approaches, in particular object relations theory, panic attacks are frequently associated with splitting (psychology), paranoid-schizoid and depressive positions, and paranoid anxiety. They are often found to be comorbid with borderline personality disorder and child sexual abuse.[74]
There was a meta-analysis of the comorbidity of panic disorders and agoraphobia that used exposure therapy to treat hundreds of patients over a period of time.[75] A result was that thirty-two percent of patients had a panic episode after treatment. They concluded that the use of exposure therapy has lasting efficacy for a client who is living with a panic disorder and agoraphobia.[75]
Medication
[edit]Medication options for panic attacks typically include benzodiazepines and antidepressants. Benzodiazepines are being prescribed less often because of their potential side effects, such as dependence, fatigue, slurred speech, and memory loss.[6] Antidepressant treatments for panic attacks include selective serotonin reuptake inhibitors (SSRIs), serotonin noradrenaline reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), and MAO inhibitors (MAOIs).[76]
SSRIs in particular tend to be the first drug treatment used to treat panic attacks. Selective serotonin reuptake inhibitors (SSRIs) and tricyclic antidepressants appear similar for short-term efficacy.[76]
SSRIs carry a relatively low risk since they are not associated with much tolerance or dependence, and have a more tolerable side effect profile. TCAs are similar to SSRIs in their many advantages but come with more common side effects such as weight gain and cognitive disturbances. MAOIs are generally suggested for patients who have not responded to other forms of treatment.[77]
While the use of drugs in treating panic attacks can be very successful, it is generally recommended that people also be in some form of therapy, such as cognitive-behavioral therapy. Drug treatments are usually used throughout the duration of panic attack symptoms and discontinued after the patient has been free of symptoms for at least six months. It is usually safest to withdraw from these drugs gradually while undergoing therapy.[27] While drug treatment seems promising for children and adolescents, they are at an increased risk of suicide while taking these medications and their well-being should be monitored closely.[77]
Prognosis
[edit]Panic attacks, while uncomfortable and scary at times, are not life-threatening but they can negatively affect one's mental health if people with recurring panic attacks do not seek treatment. Sometimes, panic attacks can develop into phobias or panic disorder if untreated. However, when treated, people do very well with symptoms decreasing or fully disappearing within several weeks to months.[78]
Epidemiology
[edit]In Europe, about 3% of the population has a panic attack in a given year. In the United States, they affect about 11%.[2] Panic attacks are more common in females than in males.[2] They often begin during puberty or early adulthood.[2] Children and older people are less commonly affected.[2] Results from twin and family studies have concluded that disorders, such as panic disorder, have a genetic component and are inherited or passed down through genes.[79]
See also
[edit]References
[edit]- ^ a b c "Anxiety Disorders". NIMH. March 2016. Archived from the original on 29 September 2016. Retrieved 1 October 2016.
- ^ a b c d e f g h i j k l m n o p q r s American Psychiatric Association (2013), Diagnostic and Statistical Manual of Mental Disorders (5th ed.), Arlington: American Psychiatric Publishing, pp. 214–217, ISBN 978-0-89042-555-8
- ^ a b Bandelow, Borwin; Domschke, Katharina; Baldwin, David (2013). Panic Disorder and Agoraphobia. OUP Oxford. p. Chapter 1. ISBN 978-0-19-100426-1. Archived from the original on 20 December 2016.
- ^ a b Craske, Michelle G; Stein, Murray B (December 2016). "Anxiety". The Lancet. 388 (10063): 3048–3059. doi:10.1016/S0140-6736(16)30381-6. PMID 27349358. S2CID 208789585.
- ^ a b "Panic Disorder: When Fear Overwhelms". NIMH. 2022. Archived from the original on 23 March 2022. Retrieved 18 March 2022.
- ^ a b Batelaan, Neeltje M.; Van Balkom, Anton J. L. M.; Stein, Dan J. (April 2012). "Evidence-based pharmacotherapy of panic disorder: an update". The International Journal of Neuropsychopharmacology. 15 (3): 403–415. doi:10.1017/S1461145711000800. hdl:1871/42311. PMID 21733234.
- ^ a b c Geddes, John; Price, Jonathan; McKnight, Rebecca (2012). Psychiatry. OUP Oxford. p. 298. ISBN 978-0-19-923396-0. Archived from the original on 4 October 2016.
- ^ Lo, Yu-Chi; Chen, Hsi-Han (May 2020). "Shiau-Shian Huang Panic Disorder Correlates with the Risk for Sexual Dysfunction". Journal of Psychiatric Practice. 26 (3): 185–200. doi:10.1097/PRA.0000000000000460. PMID 32421290. S2CID 218643956.
- ^ Smith, Melinda; Robinson, Lawrence; Segal, Jeanne. "Panic Attacks and Panic Disorder". HelpGuide. Archived from the original on 9 July 2021. Retrieved 6 July 2021.
- ^ Ghadri, Jelena-Rima; Wittstein, Ilan Shor; Prasad, Abhiram; Sharkey, Scott; Dote, Keigo; Akashi, Yoshihiro John; Cammann, Victoria Lucia; Crea, Filippo; Galiuto, Leonarda; Desmet, Walter; Yoshida, Tetsuro; Manfredini, Roberto; Eitel, Ingo; Kosuge, Masami; Nef, Holger M; Deshmukh, Abhishek; Lerman, Amir; Bossone, Eduardo; Citro, Rodolfo; Ueyama, Takashi; Corrado, Domenico; Kurisu, Satoshi; Ruschitzka, Frank; Winchester, David; Lyon, Alexander R; Omerovic, Elmir; Bax, Jeroen J; Meimoun, Patrick; Tarantini, Giuseppe; Rihal, Charanjit; Y.-Hassan, Shams; Migliore, Federico; Horowitz, John D; Shimokawa, Hiroaki; Lüscher, Thomas Felix; Templin, Christian (7 June 2018). "International Expert Consensus Document on Takotsubo Syndrome (Part I): Clinical Characteristics, Diagnostic Criteria, and Pathophysiology". European Heart Journal. 39 (22): 2032–2046. doi:10.1093/eurheartj/ehy076. PMC 5991216. PMID 29850871.
- ^ Administration, Substance Abuse and Mental Health Services (June 2016). "Table 3.10, Panic Disorder and Agoraphobia Criteria Changes from DSM-IV to DSM-5". www.ncbi.nlm.nih.gov. Retrieved 2024-10-29.
- ^ American Psychiatric Association, American Psychiatric Association. "Changes to the DSM-V to the DSM-V-TR" (PDF). Changes to the DSM V to DSM V-TR. Archived (PDF) from the original on 2 September 2018. Retrieved 22 March 2022.
- ^ Stewart, Julian M.; Pianosi, Paul; Shaban, Mohamed A.; Terilli, Courtney; Svistunova, Maria; Visintainer, Paul; Medow, Marvin S. (1 November 2018). "Hemodynamic characteristics of postural hyperventilation: POTS with hyperventilation versus panic versus voluntary hyperventilation". Journal of Applied Physiology. 125 (5): 1396–1403. doi:10.1152/japplphysiol.00377.2018. ISSN 8750-7587. PMC 6442665. PMID 30138078.
- ^ Roth, Walton T. (January 2010). "Diversity of effective treatments of panic attacks: what do they have in common?". Depression and Anxiety. 27 (1): 5–11. doi:10.1002/da.20601. PMID 20049938. S2CID 31719106.
- ^ Tully, Phillip J; Wittert, Gary A; Turnbull, Deborah A; Beltrame, John F; Horowitz, John D; Cosh, Suzanne; Baumeister, Harald (December 2015). "Panic disorder and incident coronary heart disease: a systematic review and meta-analysis protocol". Systematic Reviews. 4 (1): 33. doi:10.1186/s13643-015-0026-2. ISSN 2046-4053. PMC 4376084. PMID 25875199.
- ^ Allan, Nicholas P.; Gorka, Stephanie M.; Saulnier, Kevin G.; Bryan, Craig J. (2023-04-01). "Anxiety Sensitivity and Intolerance of Uncertainty: Transdiagnostic Risk Factors for Anxiety as Targets to Reduce Risk of Suicide". Current Psychiatry Reports. 25 (4): 139–147. doi:10.1007/s11920-023-01413-z. ISSN 1535-1645. PMC 10064604. PMID 37000403.
- ^ "Symptoms and causes - Mayo Clinic". www.mayocinic .org. Archived from the original on 17 March 2022. Retrieved 17 March 2022.
- ^ a b "Panic Disorder | Anxiety and Depression". adaa.org. Archived from the original on 12 March 2023. Retrieved 12 March 2023.
- ^ a b c d e Cackovic, Curt; Nazir, Saad; Marwaha, Raman (2024), "Panic Disorder", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 28613692, retrieved 2024-10-30
- ^ a b c Klerman, Gerald L.; Hirschfeld, Robert M. A.; Weissman, Myrna M. (1993). Panic Anxiety and Its Treatments: Report of the World Psychiatric Association Presidential Educational Program Task Force. American Psychiatric Association. p. 44. ISBN 978-0-88048-684-2.
- ^ a b c Bourne, E. (2005). The Anxiety and Phobia Workbook, 4th Edition: New Harbinger Press.[page needed]
- ^ a b c Ojha, Niranjan; Dhamoon, Amit S. (2024), "Myocardial Infarction", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 30725761, retrieved 2024-10-31
- ^ Nolen-Hoeksema, Susan (2013). (Ab)normal Psychology (6th ed.). McGraw Hill. ISBN 978-0-07-803538-8.[page needed]
- ^ Marquardt, David Z. Hambrick, Madeline (March 2018). "Bad News for the Highly Intelligent". Scientific American. Archived from the original on 27 January 2021. Retrieved 26 January 2021.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ Gregory a. Leskin, PhD (January 2004). "Gender Differences in Panic Disorder". Psychiatric Times. Psychiatric Times Vol 21 No 1. 21 (1). Archived from the original on 23 January 2021. Retrieved 26 January 2021.
- ^ Davies, Matthew N.; Verdi, Serena; Burri, Andrea; Trzaskowski, Maciej; Lee, Minyoung; Hettema, John M.; Jansen, Rick; Boomsma, Dorret I.; Spector, Tim D. (14 August 2015). "Generalised Anxiety Disorder – A Twin Study of Genetic Architecture, Genome-Wide Association and Differential Gene Expression". PLOS ONE. 10 (8): e0134865. Bibcode:2015PLoSO..1034865D. doi:10.1371/journal.pone.0134865. PMC 4537268. PMID 26274327.
- ^ a b c d Taylor, C Barr (22 April 2006). "Panic disorder". BMJ. 332 (7547): 951–955. doi:10.1136/bmj.332.7547.951. PMC 1444835. PMID 16627512.
- ^ William T. O‘Donohue,· Lorraine T. Benuto, Lauren Woodward Tolle (eds, 2013). Handbook of Adolescent Health Psychology, Springer, New York. ISBN 978-1-4614-6632-1. Page 511
- ^ "Medical marijuana and the mind - Harvard Health". Archived from the original on 21 August 2016. Retrieved 14 August 2016.
- ^ Zvolensky, Michael J.; Gonzalez, Adam; Bonn-Miller, Marcel O.; Bernstein, Amit; Goodwin, Renee D. (February 2008). "Negative reinforcement/negative affect reduction cigarette smoking outcome expectancies: Incremental validity for anxiety focused on bodily sensations and panic attack symptoms among daily smokers". Experimental and Clinical Psychopharmacology. 16 (1): 66–76. doi:10.1037/1064-1297.16.1.66. PMID 18266553.
- ^ Panic Disorder – familydoctor.org Archived 3 February 2014 at the Wayback Machine
- ^ "Anxiety Disorders" Archived 12 April 2014 at the Wayback Machine
- ^ Shin, Jin; Park, Doo-Heum; Ryu, Seung-Ho; Ha, Jee Hyun; Kim, Seol Min; Jeon, Hong Jun (2020-07-24). "Clinical implications of agoraphobia in patients with panic disorder". Medicine. 99 (30): e21414. doi:10.1097/MD.0000000000021414. PMC 7387026. PMID 32791758.
- ^ Perugi, Giulio; Frare, Franco; Toni, Cristina (2007). "Diagnosis and treatment of agoraphobia with panic disorder". CNS Drugs. 21 (9): 741–764. doi:10.2165/00023210-200721090-00004. ISSN 1172-7047. PMID 17696574. S2CID 43437233. Archived from the original on 24 February 2021. Retrieved 3 February 2021.
- ^ Bowker, Julie C.; Bowker, Matthew H.; Santo, Jonathan B.; Ojo, Adesola Adebusola; Etkin, Rebecca G.; Raja, Radhi (3 September 2019). "Severe Social Withdrawal: Cultural Variation in Past Hikikomori Experiences of University Students in Nigeria, Singapore, and the United States". The Journal of Genetic Psychology. 180 (4–5): 217–230. doi:10.1080/00221325.2019.1633618. ISSN 0022-1325. PMID 31305235. S2CID 196616453.
- ^ Teo, Alan R.; Gaw, Albert C. (June 2010). "Hikikomori, a Japanese Culture-Bound Syndrome of Social Withdrawal?: A Proposal for DSM-5". Journal of Nervous & Mental Disease. 198 (6): 444–449. doi:10.1097/NMD.0b013e3181e086b1. ISSN 0022-3018. PMC 4912003. PMID 20531124.
- ^ a b Alshak, Mark N.; Das, Joe M. (2024), "Neuroanatomy, Sympathetic Nervous System", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 31194352, retrieved 2024-11-04
- ^ a b c d e f g h Maren, Stephen (November 2009). "An Acid-Sensing Channel Sows Fear and Panic". Cell. 139 (5): 867–869. doi:10.1016/j.cell.2009.11.008. hdl:2027.42/83231. PMID 19945375. S2CID 18322284.
- ^ a b c d e Vollmer, L L; Strawn, J R; Sah, R (2015-05-26). "Acid–base dysregulation and chemosensory mechanisms in panic disorder: a translational update". Translational Psychiatry. 5 (5): e572. doi:10.1038/tp.2015.67. ISSN 2158-3188. PMC 4471296. PMID 26080089.
- ^ a b Kim, Jieun E; Dager, Stephen R; Lyoo, In Kyoon (December 2012). "The role of the amygdala in the pathophysiology of panic disorder: evidence from neuroimaging studies". Biology of Mood & Anxiety Disorders. 2 (1): 20. doi:10.1186/2045-5380-2-20. ISSN 2045-5380. PMC 3598964. PMID 23168129.
- ^ a b c d Lai, Chien-Han (2019-01-25). "Fear Network Model in Panic Disorder: The Past and the Future". Psychiatry Investigation. 16 (1): 16–26. doi:10.30773/pi.2018.05.04.2. ISSN 1738-3684. PMC 6354036. PMID 30176707.
- ^ a b c d e f Bystritsky, Alexander; Khalsa, Sahib S.; Cameron, Michael E.; Schiffman, Jason (2013). "Current Diagnosis and Treatment of Anxiety Disorders". Pharmacy and Therapeutics. 38 (1): 30–57. PMC 3628173. PMID 23599668.
- ^ Montoya, Alonso; Bruins, Robert; Katzman, Martin A; Blier, Pierre (1 March 2016). "The noradrenergic paradox: implications in the management of depression and anxiety". Neuropsychiatric Disease and Treatment. 12: 541–557. doi:10.2147/NDT.S91311. PMC 4780187. PMID 27042068.
- ^ Soares-Filho, Gastao L. F.; Arias-Carrion, Oscar; Santulli, Gaetano; Silva, Adriana C.; Machado, Sergio; Nardi, Alexandre M. Valenca and Antonio E.; Nardi, AE (31 July 2014). "Chest Pain, Panic Disorder and Coronary Artery Disease: A Systematic Review". CNS & Neurological Disorders Drug Targets. 13 (6): 992–1001. doi:10.2174/1871527313666140612141500. PMID 24923348.
- ^ a b Huffman, Jeff C.; Pollack, Mark H.; Stern, Theodore A. (2002-04-01). "Panic Disorder and Chest Pain: Mechanisms, Morbidity, and Management". The Primary Care Companion for CNS Disorders. 4 (2): 54–62. doi:10.4088/PCC.v04n0203. ISSN 2155-7780. PMC 181226. PMID 15014745.
- ^ Soares-Filho, Gastão Luiz; Mesquita, Claudio; Mesquita, Evandro; Arias-Carrión, Oscar; Machado, Sergio; González, Manuel; Valença, Alexandre; Nardi, Antonio (2012). "Panic attack triggering myocardial ischemia documented by myocardial perfusion imaging study. A case report". International Archives of Medicine. 5 (1): 24. doi:10.1186/1755-7682-5-24. ISSN 1755-7682. PMC 3502479. PMID 22999016.
- ^ "Elevated troponin linked to mental stress ischemia in heart disease patients". ScienceDaily. Retrieved 2024-04-16.
- ^ a b Rockville (MD), Substance Abuse and Mental Health Services Administration. (June 2016). "Table 3.10, Panic Disorder and Agoraphobia Criteria Changes from DSM-IV to DSM-5". www.ncbi.nlm.nih.gov. Archived from the original on 7 March 2023. Retrieved 14 March 2023.
- ^ "Panic Disorder Screener (PADIS)". ANU National Centre for Epidemiology and Population Health. Retrieved 2024-10-30.
- ^ "Panic disorder: MedlinePlus Medical Encyclopedia". medlineplus.gov. Archived from the original on 8 June 2023. Retrieved 12 March 2023.
- ^ a b Manjunatha, Narayana; Ram, Dushad (March 2022). "Panic disorder in general medical practice- A narrative review". Journal of Family Medicine and Primary Care. 11 (3): 861–869. doi:10.4103/jfmpc.jfmpc_888_21. ISSN 2249-4863. PMC 9051703. PMID 35495823.
- ^ Susman, Jeffrey; Klee, Brian (2005-02-15). "The Role of High-Potency Benzodiazepines in the Treatment of Panic Disorder". The Primary Care Companion for CNS Disorders. 7 (1): 5–11. doi:10.4088/PCC.v07n0101. ISSN 2155-7780. PMC 1076453. PMID 15841187.
- ^ Generalised anxiety disorder and panic disorder in adults: management. Clinical Guideline 113. National Institute for Health and Care Excellence. 26 July 2019. ISBN 978-1-4731-2854-5. Archived from the original on 22 November 2018. Retrieved 8 January 2021.
- ^ Bandelow, Borwin; Seidler-Brandler, Ulrich; Becker, Andreas; Wedekind, Dirk; Rüther, Eckart (January 2007). "Meta-analysis of randomized controlled comparisons of psychopharmacological and psychological treatments for anxiety disorders". The World Journal of Biological Psychiatry. 8 (3): 175–187. doi:10.1080/15622970601110273. PMID 17654408. S2CID 8504020.
- ^ Correll, Terry; Gentile, July; Correll, Andrew (September 1, 2023). "Healthy Lifestyle Interventions Augmenting Psychotherapy in Anxiety and PTSD". Innovations in Clinical Neuroscience. 20 (7–9): 18–26. PMC 10561983. PMID 37817811.
- ^ Chong, Terence W. H.; Curran, Eleanor; Southam, Jenny; Bryant, Christina; Cox, Kay L; Ellis, Kathryn A.; Anstey, Kaarin J.; Goh, Anita; Lautenschlager, Nicola T (2023-12-01). "The potential of physical activity and technology interventions to reduce anxiety in older adults". Journal of Affective Disorders Reports. 14: 100633. doi:10.1016/j.jadr.2023.100633. ISSN 2666-9153.
- ^ "3 Tips for Using Exercise to Shrink Anxiety". 17 July 2013. Archived from the original on 20 April 2015. Retrieved 14 April 2015.[full citation needed]
- ^ MedlinePlus Encyclopedia: Hyperventilation
- ^ "Cardio Exercise for Beginners". Archived from the original on 23 April 2015. Retrieved 14 April 2015.[full citation needed]
- ^ Klevebrant, Lisa; Frick, Andreas (2022). "Effects of caffeine on anxiety and panic attacks in patients with panic disorder: A systematic review and meta-analysis". General Hospital Psychiatry. 74: 22–31. doi:10.1016/j.genhosppsych.2021.11.005. ISSN 1873-7714. PMID 34871964.
- ^ American Psychiatric Association. (2000). Diagnostic and statistical manual of mental disorders (4th ed., text rev., p. 479). Washington, D.C.: American Psychiatric Association.[page needed]
- ^ Kabat-Zinn, J; Massion, AO; Kristeller, J; Peterson, LG; Fletcher, KE; Pbert, L; Lenderking, WR; Santorelli, SF (July 1992). "Effectiveness of a meditation-based stress reduction program in the treatment of anxiety disorders". American Journal of Psychiatry. 149 (7): 936–943. CiteSeerX 10.1.1.474.4968. doi:10.1176/ajp.149.7.936. PMID 1609875.
- ^ a b c Banushi, Blerida; Brendle, Madeline; Ragnhildstveit, Anya; Murphy, Tara; Moore, Claire; Egberts, Johannes; Robison, Reid (2023-02-02). "Breathwork Interventions for Adults with Clinically Diagnosed Anxiety Disorders: A Scoping Review". Brain Sciences. 13 (2): 256. doi:10.3390/brainsci13020256. ISSN 2076-3425. PMC 9954474. PMID 36831799.
- ^ "Hyperventilation Syndrome". 28 November 2016. Archived from the original on 13 July 2017. Retrieved 18 September 2017.
- ^ Craske, Michelle (30 September 2011). "Psychotherapy for panic disorder". Archived from the original on 14 October 2017. Retrieved 29 April 2020.
- ^ Meuret, Alicia E.; Ritz, Thomas (October 2010). "Hyperventilation in panic disorder and asthma: Empirical evidence and clinical strategies". International Journal of Psychophysiology. 78 (1): 68–79. doi:10.1016/j.ijpsycho.2010.05.006. PMC 2937087. PMID 20685222.
- ^ Bhagat, Vidya; Haque2, Mainul; Jaalam3, Kamarudin (2017). "Breathing Exercise - A Commanding Tool for Self-help Management during Panic attacks". Research Journal of Pharmacy and Technology, 10(12), 4471-4473. 10 (12): 4471–4473.
{{cite journal}}: CS1 maint: numeric names: authors list (link) - ^ Breathing in and out of a paper bag Archived 21 October 2007 at the Wayback Machine
- ^ Bergeron, J. David; Le Baudour, Chris (2009). "Chapter 9: Caring for Medical Emergencies". First Responder (8 ed.). New Jersey: Pearson Prentice Hall. p. 262. ISBN 978-0-13-614059-7.
Do not use a paper bag in an attempt to treat hyperventilation. These patients can often be cared for with low-flow oxygen and lots of reassurance
- ^ Hyperventilation Syndrome – Can I treat hyperventilation syndrome by breathing into a paper bag? Archived 20 January 2013 at the Wayback Machine
- ^ "Answers to Your Questions About Panic Disorder". American Psychological Association. 2008. Archived from the original on 10 January 2021. Retrieved 8 January 2021.
- ^ Cramer, K., Post, T., & Behr, M. (January 1989). "Cognitive Restructuring Ability, Teacher Guidance and Perceptual Distracter Tasks: An Aptitude Treatment Interaction Study". Archived from the original on 22 December 2010. Retrieved 19 November 2010.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ Abramowitz, Jonathan S.; Deacon, Brett J.; Whiteside, Stephen P. H. (17 December 2012). Exposure Therapy for Anxiety: Principles and Practice. Guilford Press. ISBN 978-1-4625-0969-0. Archived from the original on 20 May 2016.
- ^ Waska, Robert (2010). Treating Severe Depressive and Persecutory Anxiety States: To Transform the Unbearable. Karnac Books. ISBN 978-1855757202.[page needed]
- ^ a b Fava, G. A.; Rafanelli, C.; Grandi, S.; Conti, S.; Ruini, C.; Mangelli, L.; Belluardo, P. (July 2001). "Long-term outcome of panic disorder with agoraphobia treated by exposure". Psychological Medicine. 31 (5): 891–898. doi:10.1017/s0033291701003592. PMID 11459386. S2CID 5652068.
- ^ a b Bakker, A.; Van Balkom, A. J. L. M.; Spinhoven, P. (2002). "SSRIs vs. TCAs in the treatment of panic disorder: a meta-analysis". Acta Psychiatrica Scandinavica. 106 (3): 163–167. doi:10.1034/j.1600-0447.2002.02255.x. PMID 12197851. S2CID 26184300.
- ^ a b Marchesi, Carlo (March 2008). "Pharmacological management of panic disorder". Neuropsychiatric Disease and Treatment. 4 (1): 93–106. doi:10.2147/ndt.s1557. PMC 2515914. PMID 18728820.
- ^ "Panic attacks and panic disorder - Diagnosis and treatment - Mayo Clinic". www.mayoclinic.org. Retrieved 2024-11-14.
- ^ Hettema, John M.; Neale, Michael C.; Kendler, Kenneth S. (October 2001). "A Review and Meta-Analysis of the Genetic Epidemiology of Anxiety Disorders". American Journal of Psychiatry. 158 (10): 1568–1578. doi:10.1176/appi.ajp.158.10.1568. PMID 11578982. S2CID 7865025.
